GERD and Oral Health
Gastroesophageal reflux disease can affect teeth and gums
Dear Doctor,
My father was just diagnosed with GERD, which was first noticed by his dentist. Can you tell me more about this condition and why it would affect his teeth?
Dear Hadley,
It’s actually not surprising that your father’s dentist was the first to discover signs of gastroesophageal reflux disease, or GERD. Though it is a digestive condition, GERD can damage teeth and gums by allowing powerful stomach acids to flow back up the digestive tract and into the mouth. It can also cause other health problems.
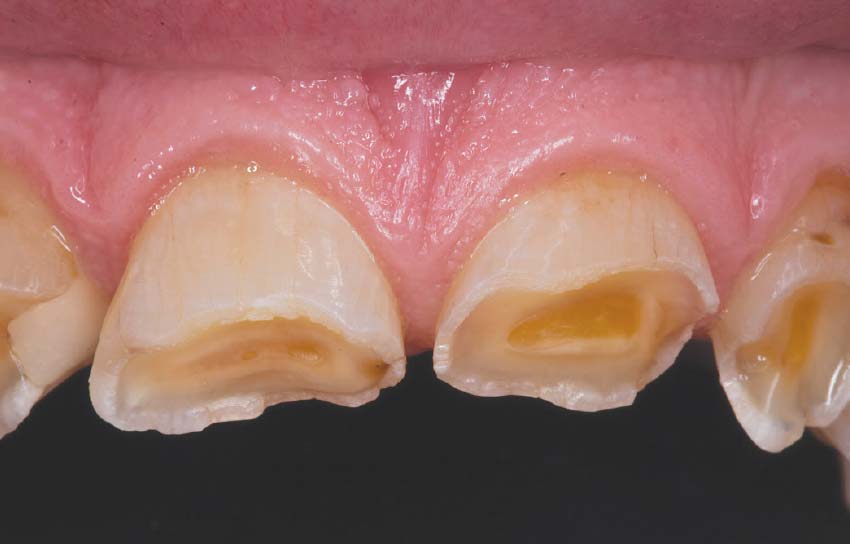 |
| Stomach acid is strong enough to break down food, and can cause serious damage to your teeth. |
Most people have experienced at least occasional acid reflux or heartburn—perhaps after eating too much or after eating certain foods. When the painful, burning sensation caused by stomach acids flowing backwards occurs at least twice a week, it is usually diagnosed as GERD. This medical condition affects approximately 1 in 5 US adults. For many, GERD symptoms make life miserable; for others who have more subtle symptoms, or no symptoms at all (“clinically silent reflux”), chronic acid reflux may go undiagnosed. Yet over time, untreated GERD can damage the lining of the esophagus, causing ulcers and pre-cancerous cells to develop, a condition called “Barrett’s Esophagus.” GERD also has potentially serious consequences for oral health: Repeated acid reflux can eat away at the teeth and damage the gums. That’s why dentists sometimes notice signs of this condition during a routine oral exam.
How Acid Affects Your Teeth
A ring of muscle at the bottom of the esophagus called the lower esophageal sphincter acts as a one-way valve to keep stomach contents from moving back up the digestive tract. But when this muscle is weak or damaged, stomach acids can flow up into the esophagus and even enter the mouth. As stomach contents flow backwards, a burning sensation in your chest or throat—heartburn and acid indigestion—may result.
A prominent sign of GERD is tooth erosion, a breakdown of a tooth’s protective outer coating (enamel) caused by acid washing up into the mouth. On the pH scale, which measures acidity, a normal, heathy oral pH is around 7.0 (the same as pure water). A more acidic pH of 5.5 or lower begins to dissolve tooth enamel. Stomach acid, with a pH of 2.0 or less, is strong enough to break down food, and is also capable of causing serious dental damage.
Unfortunately, you may not notice how GERD affects your oral health until severe damage has been done. Erosion from GERD is most frequently seen on the inside surfaces of upper teeth. Teeth can become thin, sharp, chipped, pitted, yellow and sensitive, requiring extensive—and expensive—dental work. A lower salivary pH can also damage soft tissues of the mouth, and is linked to periodontal (gum) disease. A 2014 study found a strong correlation between GERD and chronic periodontitis, an inflammation of the gums and other supporting structures of the teeth that may cause bone loss. Periodontitis can also cause teeth to become loose and eventually fall out.
Even people who experience more subtle symptoms of GERD can have dental erosion and gum disease, so dentists can be key players in identifying the condition and getting people on the path to treatment.
Protecting Your Teeth
You can do your part in protecting your teeth from the effects of acid reflux. Here are some suggestions:
- To stimulate saliva production, chew sugar-free xylitol gum. Saliva helps neutralize acid and contains minerals that help build the tooth surface. Although all chewing gum stimulates saliva, gum with the sugar substitute xylitol also interferes with the chemical reaction between acid and tooth structure, thus reducing calcium loss.
- Refrain from brushing your teeth right after an acid reflux episode. Acid softens tooth enamel, so wait an hour to give your saliva a chance to wash out the acid and to build the minerals in the teeth back up.
- Instead, after a reflux episode, rinse your mouth out with water.
- To neutralize the acid, mix half a teaspoon of baking soda into a cup of water and rinse, or chew on an antacid tablet or rinse with antacid suspension. Sugar-free forms of antacids are best.
- To strengthen your teeth, ask your dentist about fluoride toothpaste, special mouth rinses or in-office treatments. Toothpastes that contain ACP (amorphous calcium phosphate) can also be beneficial in preventing erosion.
- If you suffer from xerostomia (dry mouth), use a saliva substitute or chew green tea gum, which can increase saliva flow and reduce acidity in the mouth.
Lifestyle changes can also be helpful in controlling the uncomfortable symptoms of GERD. These include: avoiding alcohol, caffeine and spicy and/or acidic foods and beverages; eating smaller meals; finishing meals three hours before bedtime; and avoiding lying down right after eating. Quitting smoking and losing weight can help you avoid the symptoms of GERD, and will also benefit your overall health.
In addition, your doctor may recommend an over-the-counter or prescription medication to treat GERD or its symptoms. Be sure to tell your dentist about any medications you are taking or health conditions you have—even those you wouldn’t necessarily think of as oral health issues.
As our discussion of GERD shows, health conditions in other parts of the body can impact your oral health in significant ways. Prompt diagnosis and treatment of GERD can not only stave off serious oral health problems and costly dental work—it can also prevent other negative health effects. Since acid reflux takes its toll on the oral cavity, treatment often involves a dental professional; however, the underlying cause of this condition must also be addressed to safeguard your general health.

