Dental Implants
Your Third Set of Teeth
(Continued)
Implant placement requires planning and will involve collaborative efforts between the implant surgeon, dentist and laboratory technician.
Innovations from Clinical Practice
Clinical use and research have led to modifications of implant design and improvements such as the following:
- Improved surface characteristics — from the initial smooth and polished surfaces to the current, acid etched sandblasted, nanotech surfaces. This technical advance significantly increases the microscopic surface area of implants and thereby markedly improves the degree of attachment to bone. This also increases the success rates of osseo-integration, even where bone quality is less dense.
- Improved shapes and sizes for different tooth size replacements — Implants are made in different widths which together with improved surface characteristics provide for maximum bone to implant contact. They can therefore more easily carry the same forces as are applied to natural teeth. For example, back molar teeth have one or more roots to withstand higher biting forces necessary for chewing. Implants have likewise been developed to mirror these functions. Teeth in different areas of the mouth are designed differently to accommodate different functions.
- Improvements in design for aesthetics — connections from implants to crowns have improved to make the teeth look perfectly natural as they emerge from the gum tissues to mimic natural teeth exactly. Materials used are essentially the same as for regular crowns to imitate natural aesthetics, function and durability. Crowns are either directly connected to the implants themselves by tiny invisible screws in the back non-visible parts of the teeth, or are cemented over little tooth like receptors just like regular crowns.
Implant Treatment — A Collaborative Approach to Treatment
Normally implants are placed by periodontists and oral surgeons, dental specialists who have undertaken training in implantology and surgery as part of their training. Implant placement requires planning and will involve collaborative efforts between the implant surgeon, dentist and laboratory technician who are responsible for building a crown on a successfully integrated implant.
Diagnostic Steps
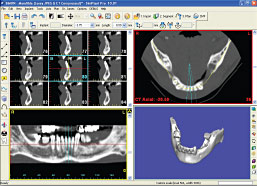 |
| Figure 1: CAT scan technology provides dentistry with images that allow for proper implant placement and safety. |
| Photo courtesy of Materialise Dental Inc. |
Your dentist and/or surgeon will follow routine procedures to assess your medical status and general health; carefully examine your mouth and the site where the potential implant or implants are to be placed; make study models of your mouth to assess your bite; take photographs if there is an aesthetic concern; take special radiographs (x-rays) of the site to assess bone quantity and quality; make surgical guides or templates to ensure accurate surgical implant placement. A discussion of all the risks, benefits and alternatives of placing implants in your particular case should take place with you and your dental “team.”
Implant Positioning
Sometimes described as “top down treatment planning,” providing that your bite is pretty functional and other teeth are aligned correctly, the teeth to be replaced are recreated in a wax model form. The idea is then to establish the position of the underlying bone and to make sure implant(s) can be positioned directly under the wax tooth form (top) to the implant, (down) beneath. The implant positions can then be predetermined using a combination of specialized radiographs (x-rays) and imaging technology [Fig. 1] to assure success and in the process avoid major structures like nerves and air sinuses. From this information surgical guides are fabricated to assist the surgeon in precise implant placement which in turn assures the restorative dentist that a crown will fit in the right position. If the bite will not accommodate implant placement orthodontic (braces) treatment may be necessary to reposition teeth, or bone may need to be regenerated surgically.
Surgical Placement
Dental implant surgery is a relatively comfortable procedure usually carried out under local anesthesia (numbing the area where the implant is to be placed), sometimes with the assistance of oral medication or intravenous conscious sedation for anxious patients. Some minor vibration is generally experienced during the implant (bone) site preparation, but it is quite tolerable. Since there are no open wounds following the surgery and it is minimally invasive, there is little post-operative discomfort, perhaps a day or two. The implant(s) need to be left for a period of 2-6 months to fuse or integrate with the bone in most circumstances. The healing time depends upon the bone density of the site, the more dense the bone, the quicker the integration. When the implant has integrated with the bone a crown can be made and the implant “loaded” that is, subjected to biting forces. Following successful integration your dentist will make a crown which fits on the implant and will be exactly like a normal tooth both in form and function.

