Tooth Removal For Orthodontic Reasons
Bone Sets The Tone For Successful Treatment
Dear Doctor,
My teenage son recently saw an orthodontist who recommended that two teeth be removed prior to braces, plus a front tooth (damaged as a result of injury). How will this increase my son's chances of successful orthodontic treatment?

Dear Mary,
This is a complicated question with multiple elements, so let's try to break it down into understandable parts.
Which Teeth And Why
The first important phase of orthodontic treatment (“ortho” – to straighten, “dont” – tooth) is figuring out what needs to be done. Treatment often involves removing teeth to relieve crowding. Generally speaking, when there are too many teeth for the size of the dental arches (upper and/or lower jaws), there may not be enough space to align them. A common solution is to create the necessary space by removing teeth to allow the others to be aligned correctly. Conversely, where a front tooth has to be replaced and there is already adequate room for it, the space has to be maintained (to prevent other teeth from moving into it), until it can be replaced with a properly sized tooth.
The teeth most frequently removed for orthodontic reasons are the first bicuspid (premolar) teeth. These are the teeth right between the cuspid or eyeteeth (under the eyes) and the molar teeth (the biggest back teeth). In some cases premolar teeth can be removed without sacrificing future cosmetics or function.
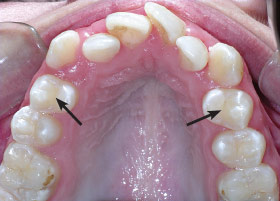 |
| Due to significant crowding, extraction of the first premolars is necessary to properly align the remaining teeth. |
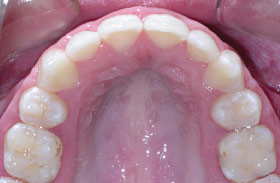 |
| Orthodontics completed with the second premolars moved into the first premolar spaces and the front teeth properly aligned. |
| Photos provided by Dr. Richard G. Rosenbloom |
Preserving Bone For Moving Teeth
Bone is a living tissue that continually reshapes itself in response to the stimulus of biting force or stress. Bone that normally supports the teeth slowly resorbs when the teeth are lost. Sometimes, if the bony housing surrounding a tooth is very thin, significant bone loss can occur after extraction. This process happens in just a matter of months, but can continue if steps are not taken to stop it. The surgeon removing a tooth may recommend a bone graft to preserve the socket bone if he is concerned that there will be too much bone loss. The reason for this consideration is that if there is insufficient bone through which to move the teeth, it can result in unsightly gum recession and root exposure following orthodontic treatment. Thus bone preservation following tooth extraction is critical to ensure that there is enough bone mass through which to move neighboring teeth for proper alignment.
Removing Teeth While Preserving Bone
Believe it or not, there is a real art and “feel” to tooth removal, and in experienced hands it can and should be done very carefully and atraumatically (“a” – without; “trauma” – damage). If you think of a tooth socket like an empty ice-cream cone, it is quite easy to collapse, especially where the bony walls are thinnest. This is especially so on the facial surfaces (the surfaces facing the cheeks and lips), where gum recession is likely to show.
Fortunately, years of evidence-based research has led to modern surgical techniques that allow for maintenance of bone mass and volume in extraction sockets. This is most often accomplished as mentioned by atraumatic surgical techniques, and in some cases, bone grafting. In fact, placing a small amount of bone grafting material (most often processed bone safe for human use), just enough to fill the empty socket, acts as a scaffold upon which the body builds its own bone, eventually replacing the grafted material.
There's another important consideration to keep in mind in your son's case: Some of the bone supporting his front tooth may already have been lost or damaged as a result of his injury. Regeneration can be facilitated with bone grafting and specialized synthetic membranes. The membranes, supported by bone grafting material, can be used as scaffolds to rebuild the bone in a socket shape. And better yet, with today's biotechnology, both graft and membrane are replaced with healthy bone, and the self-dissolving membranes don't have to be removed.
More About Bone — Planning For Future Tooth Replacement
Lastly, tooth extractions have implications for restorative dentistry (replacing lost or missing teeth) that involve tooth-supporting jawbone. In addition to maintaining the bone volume and density, it may be necessary to create or maintain space for a new tooth. This can be done with a dental implant, fixed (non-removable) bridgework, or (removable) partial denture. It is therefore important to plan for space, creating enough room and then maintaining it until the missing tooth is replaced. That way, whatever prosthesis (false tooth replacement) is chosen, it will look like it is natural and belongs there.
As they say in scuba diving — plan the dive, and then dive the plan. Your dental team needs to plan your son's case from beginning to end with the goals and sequence of tooth removal in mind. As I hope you can see, it really can be the bone that sets the tone for an aesthetic and functional final result.

