The Future of Dental Care in America
Big Changes on the Horizon
 |
Did you know that approximately one third of the U.S. population receives no dental care? That’s because access to care is the major issue facing the public today, and it’s a problem for the dental profession too. As a result, too many of our citizens are showing up at hospital emergency rooms for infections that could have been treated at a dental office. In the past year alone, almost 900,000 people went to emergency rooms for dental reasons. Meanwhile, emergency room care can cost ten times as much as a dental office visit. Often patients are sent home with pain pills and antibiotics but with no actual dental care that treats what’s causing their problems. Clearly, we need to get dental treatment — and preventive care — to more people on a regular basis. But how can we meet this urgent need? And will the practice and financing of dental care have to change in order to do it? The short answer is yes.
We’ve done a lot of research into what the barriers to care are, and the largest are financial, geographical, political and educational.
- Financial — too many people just cannot afford dentistry or they cannot afford to miss work to get to a dentist.
- Geographical — too many rural areas do not have enough dentists.
- Political — we need better public health advocacy. Government health policy needs to encourage preventive measures through municipal water fluoridation and resist misguided anti-fluoridation efforts. Public school preventive programs need to be expanded and can be a positive force to reduce sugar consumption, which affects not only oral but, importantly, general health as well.
- Educational — some people have a difficult time processing oral health information.
We know how to prevent dental disease almost completely, and there’s so much that can be done to improve oral health outside of the dental chair. That includes embracing the personal responsibility to pursue habits of good oral hygiene and healthy dietary practices.
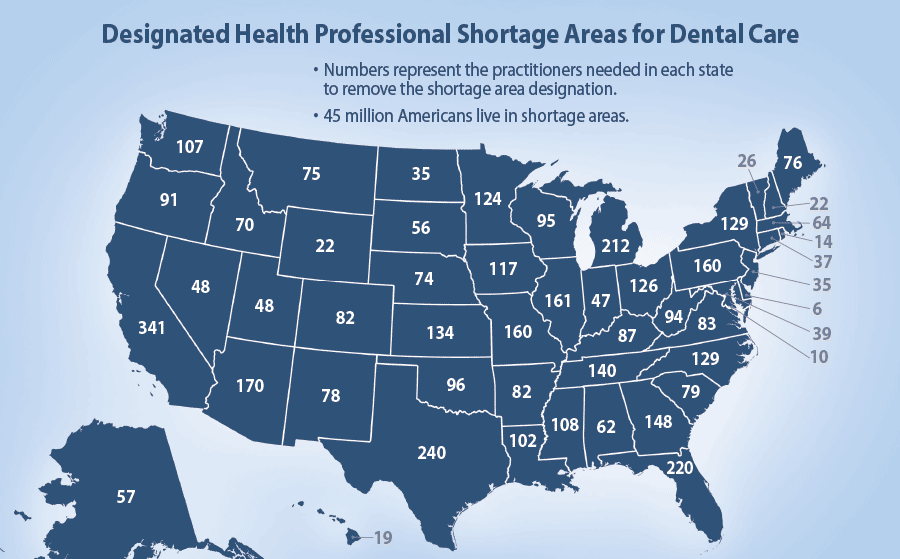 |
| Source: Bureau of Clinician Recruitment and Service, Health Resources and Services Administration (HRSA), U.S. Department of Health & Human Services, HRSA Data Warehouse: Designated Health Professional Shortage Areas Statistics, as of April 28, 2014.
Click to enlarge |
The Affordable Care Act (ACA), also known as “Obamacare,” is projected to help increase access to both medical and dental care. The American Dental Association estimates that under the ACA, 3 million children are expected to get some form of dental benefits by 2018. Since the program is just starting (with an uneven beginning) it is hard to say whether those projections will come true. Yet as much as it is talked about, the Affordable Care Act is not the only force for change in the healthcare arena — or even the biggest one. In dentistry, I see three areas in which major transformations are taking place right now.
The first is a technological change. There is going to be increased utilization and reliance on digital technology in the dental office. From a clinical perspective we have seen some exciting developments in recent years: 3-D digital scanning technology that can give dentists amazingly detailed views of both hard (bone, teeth and jaws) and soft tissues (gums and oral membranes) of the mouth; digital impressions that use a scanning wand to create virtual models of the teeth, rather than a physical model made with putty-like impression materials placed in the mouth; and lasers, which often cause less discomfort than scalpels or drills. Office computerization for digitizing patient records and communicating with dental laboratories and insurance companies is also streamlining dental management. CAD/CAM (Computer Aided Design/Computer Aided Manufacturing) technology is also being used to mill crowns and other restorations that are placed in the mouth.
Tele-dentistry is on the horizon and is currently being studied in pilot programs. A dentist will be able to review dental x-rays and diagnose dental conditions via a video camera and computer. The dental care may be delivered by dental hygienists and dental assistants trained to perform certain basic procedures that only dentists do now, such as placing temporary fillings. This could stabilize decayed teeth until a visit to a dentist is arranged. This would cut costs and prevent hospital emergency room visits while improving access to care, especially in areas of dental manpower shortages like remote areas. But it will be important to make sure these auxiliary staff members are appropriately supervised.
The second is a change in the way dental services are delivered. There will be fewer and fewer solo practitioners of dentistry. Consider this: The cost of dental education is very high. When a young dentist comes out of school, he or she will often be $300,000 to $500,000 in debt. Setting up a private practice can take another $500,000 — the high-tech equipment mentioned above being just part of the necessary investment. That means a dentist just starting out in private practice may be up to $1 million in debt before earning their first dollar! It’s no wonder that more dentists are opting to work in larger group settings where expenses are shared or for dental corporations, which relieve them of the financial responsibility for setting up a practice.
There are many new models of dental practice that are emerging as a result. For example dental corporations have formed, some run by dentists and some run by investment bankers that provide management services and free the dentists to do just clinical dentistry. But which is better for the patient — a small solo practice or a large group or corporate practice? There are advantages and disadvantages to both. A positive aspect to a large, group practice is that you can have many dentists in one location performing the procedures at which they’re most skilled; and specialists can interact more easily with general dentists when under one roof. The downside can be a lack of personal interaction with one provider. You may not be able to build a relationship over many years with one dentist who really becomes your dentist. So it’s often a mixed bag.
Increased pressure for cost-cutting will also come from insurance companies. There is a downward pressure on fees by the major insurance carriers. Also, there is pressure to move away from paying a set fee for a particular service — say, a filling or crown — and towards a system of payment based on improved longer-term outcomes of treatment. The healthier a person or a community remains for the least amount of care that is needed, will be what is rewarded. This changes the incentive away from treatment and towards prevention. The goal is to cut costs while helping the patient stay healthy. You’re going to see different approaches tried to achieve that.
A third area of change will be greater collaboration between physicians and dentists. Dentists will start to do more diagnostic medical procedures, such as screening for cancer and diabetes. This will be made possible by fascinating recent developments in the field of salivary diagnosis. Scientists are finding more and more ways to test for serious diseases using saliva instead of blood. We’ll see a lot of dentists doing this, because many people see their dentists more regularly than they see their physicians. Increasing opportunities for early disease detection and intervention will help control costs and increase health outcomes in the long run to the benefit of patients. After all, the best way to make sure people get all the care they need is to prevent them from needing very much at all.



