Orofacial Myofunctional Therapy
How retraining oral and facial muscles can benefit your bite
 |
Think of a healthy mouth and the first image that comes to mind may be a pearly-white smile. But while teeth may be the mouth’s most noticeable feature, they are only one part of the picture. Helping a smile look its best—or treating a problem in the oral cavity—often goes beyond the teeth. Many health care professionals bring their expertise to this area, including dentists and dental specialists (periodontists, orthodontists, oral surgeons, etc); ear nose and throat specialists; speech pathologists; and orofacial myologists.
If you’ve never heard of that last one, you’re not alone—yet thousands of people benefit from seeing these specialists every year, often at the suggestion of their dentists. So what exactly is orofacial myology? It is the study and treatment of the oral and facial muscles as they relate to speech, dentition (teeth), chewing and swallowing, and overall health.
Youngsters who have just had orthodontic treatment, for example, may be referred to an orofacial myologist to help preserve their newly straightened smiles; dentists may recommend treatment for children who show signs of persistent thumb sucking; pediatricians may notice evidence of continual mouth breathing; and parents may observe speech or eating problems that could be corrected with Orofacial Myofunctional Therapy (OMT). According to the International Association of Orofacial Myology, some 38% of the general population and 81% of kids with speech problems have an orofacial myofunctional disorder. These disorders can often be addressed via the non-invasive treatment methods of OMT.
The field may be best known for treating the problem of “tongue thrusting,” a potentially harmful habit where the tongue is forced against (or between) the front teeth during swallowing. Over time, this can lead to troublesome orthodontic problems. Yet OMT is concerned with more than just swallowing—an activity performed for a total of perhaps 20-30 minutes every day. It also addresses how the mouth functions when it is at rest—much of the remaining 23½ hours. Recent studies have shown that a poor mouth resting posture, where the tongue rests low in the mouth, causes the teeth to shift.
The Mouth at Rest
In a normal, relaxed posture—while sitting down and reading, for example—the mouth is closed and the top and bottom teeth don’t touch. The tip of the tongue rests on the upper palate, about 5 mm behind the front teeth. There is usually a vertical gap of 2-3 mm between the molars in back, and 4-6 mm between the incisors in front. This open resting space is called the freeway space or interocclusal (inter – “between”; occlusion – “bite”) space. Breathing is done through the nose.
In people with orofacial myofunctional disorders (OMDs), the vertical dimension of the freeway space is outside the normal range. When excessive space is present, over time the teeth can erupt (emerge from the gums) too much, or in unwanted positions. Poor positioning of the tongue causes the front teeth eventually to be pushed out of alignment, and may alter the shape of the bite. These problems, often noticed in children, are called malocclusions (mal – “bad”; occlusion – “bite”). The opposite problem, too little space, may become apparent when teeth are not in proper position, but instead stick out of the normal alignment.
In many instances, a general dentist or orthodontist will be the one who refers a patient to an orofacial myologist. This may be to help correct a parafunctional (“para” – irregular; “function” – operation) habit like thumb or finger sucking, or to ensure that teeth stay in their improved positions after orthodontic treatment. Many orthodontists refer patients before treatment begins in order to ensure a better result or to get a second opinion regarding timing of expansion or placement of retainers. Thumb and finger sucking habits need to be resolved before orthodontic treatment. Studies have shown that in conjunction with orthodontics, OMT is an effective treatment for malocclusions such as “open bite.” Let’s take a closer look at how the facial muscles and the tongue may affect these conditions.
Tongue Thrusting and Open Bite
The behavioral pattern called “tongue thrusting” is a problem often found in children. It generally occurs when there is too much freeway space while the mouth is at rest—a problem that can be caused by many factors. Airway obstructions (such as enlarged tonsils/adenoids or allergies that cause mouth breathing), low tongue posture, and/or tongue and lip ties (ankyloglossia) all contribute to low tongue posture, as well as the creation of abundant freeway space. The tongue adapts to this situation by moving forward against the teeth; it may also be thrust into the gap between the front teeth while swallowing, creating a seal that prevents food or drinks from escaping from the mouth. This behavior, called the “infantile swallowing pattern,” is normal in babies, but is usually replaced by the adult pattern by age four. (In fact, we see adult patterns as early as age 2 but children can go through many different patterns until age 10). If it persists much beyond that age, it may signal trouble.
 |
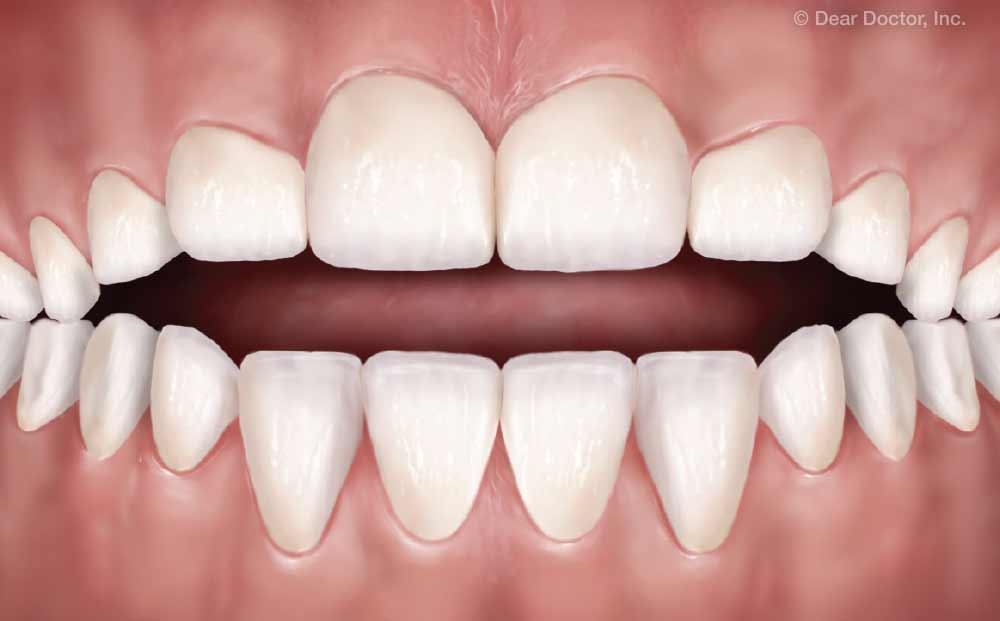 |
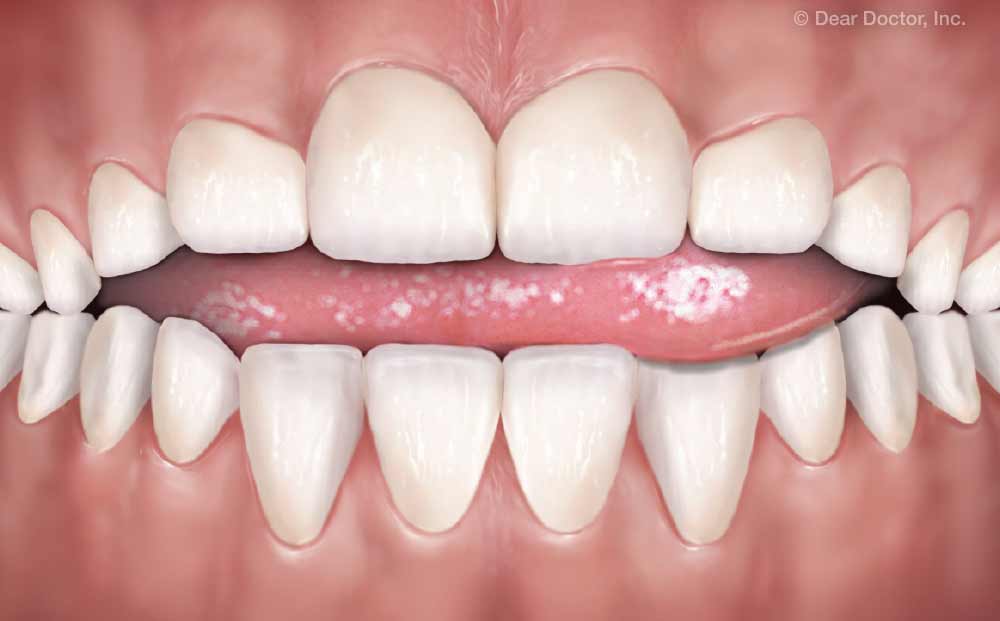
| In a normal relaxed posture (bottom), when the mouth is closed, there is a gap between the top and bottom front teeth of 4-6mm, and the tip of the tongue rests on the upper palate (the roof of the mouth). In the behavioral pattern called “tongue thrusting” (top), the tongue moves too far forward, and may be thrust into the gap between the front teeth. |
An open bite occurs when the front teeth, instead of meeting or overlapping, are separated by the constant presence of the tongue or are pushed outward; they do not close the space in front of the mouth. At one time it was thought that the brief, intense pressure produced by tongue thrusting during swallowing actually moved the front teeth forward. However, studies using tiny pressure sensors in children’s mouths have shown just the opposite: It’s the constant slight pressure of the tongue, pushing against the front teeth while at rest, that moves teeth out of line—in much the same way that braces use a steady, light force to move teeth into better positions.
From the perspective of orofacial myology, tongue thrusting isn’t the cause of orthodontic trouble; the behavior is an adaptation to the extra freeway space—an oral problem that’s already there. That’s why OMT does not employ appliances such as “tongue cribs” to physically prevent the tongue from pushing on the teeth; instead, orofacial myologists seek to retrain the tongue to develop better habits.
How Orofacial Myofunctional Therapy Works
Orofacial myofunctional therapy uses muscular exercises, positive reinforcement and motivational techniques to achieve the desired result: an improved rest posture of the mouth, with proper tongue position and nasal breathing instead of mouth breathing. OMT isn’t a one-size-fits-all treatment; it is tailored to an individual’s age, ability and needs, with different techniques used as appropriate. In general, however, treatment is divided into three phases. The first uses exercises to get the tongue up to the proper spot on the palate, and to maintain proper muscle tone and lip strength. The second involves getting the tongue and mouth to perform the normal swallowing pattern. In the third phase, we help people get comfortable with using their newly learned behaviors every day.
 |
| Performing OMT exercises in front of a mirror gives important visual feedback |
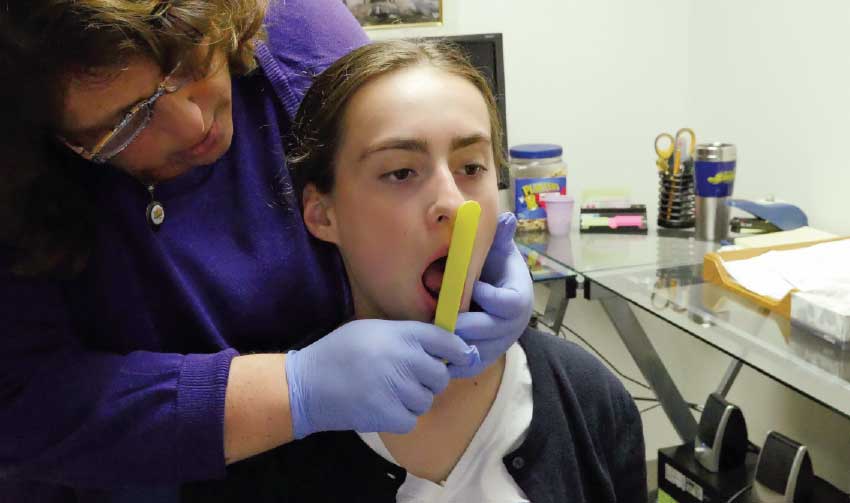 |
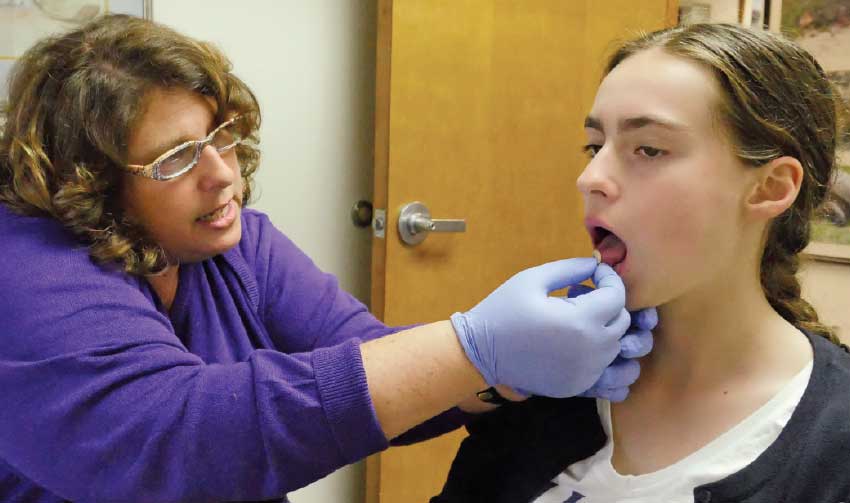
| Therapists use simple tools to assist patients with tongue placement and range of motion |
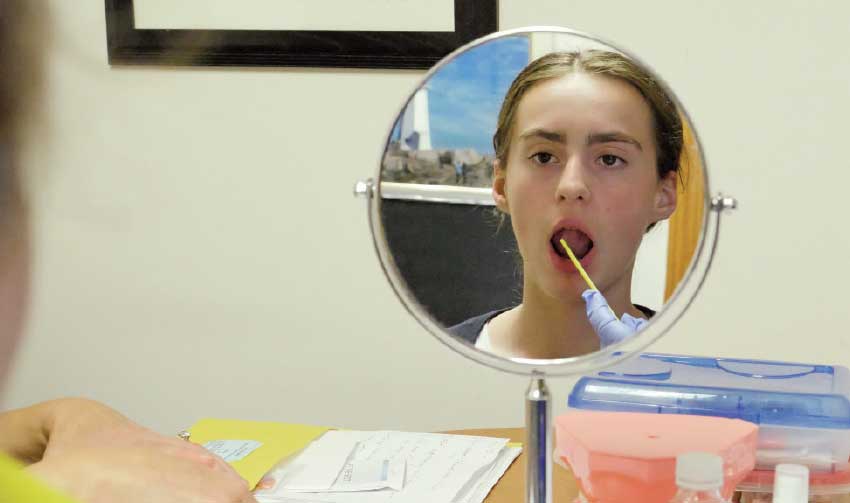 |
| A tongue depressor provides tactile cues that can help improve oral posture |
 |
| A Cheerio or dental elastic is often used to guide the tongue to the correct spot on the palate |
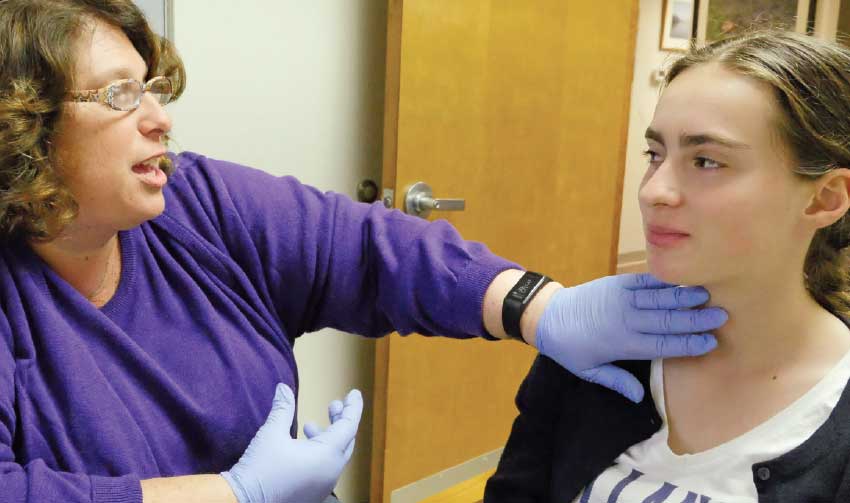 |
| Patients learn that the tongue, rather than the neck muscles, should be the main player in swallowing |
Many of the exercises we do are practiced in front of a mirror so it’s easier to see what’s happening. We often ask the patient to have a partner, whether the patient is a child or an adult; children greatly benefit from parental involvement. We use simple tools such as tongue depressors, coffee stirrers, Cheerios and/or dental elastics in order to give patients good cues during exercises. Everyone likes the later swallowing exercises since they involve eating a snack!
Positive reinforcement is a major element we use to motivate people. It isn’t always easy to change an ingrained habit, but with cooperation, commitment and an occasional reward, we can be successful. Depending on the individual, that might be a colorful sticker, a mani/pedi appointment in the case of decreased thumb or finger sucking, or a small gift. It might also be seeing a more pleasing smile in the mirror, eating without losing food from the mouth, or waking up with a pillow that isn’t damp with saliva from sleeping with an open mouth.
Yet habits that are formed over time also take time to correct. With OMT, we generally see improvement over a period of weeks, and expect to finish therapy in a few months; from beginning to end, there may be 15-17 sessions. During that time, an orofacial myologist may act like a coach, a teacher, and a cheerleading section. We rely on the active participation of our patients: Ultimately, our goal is to help them change their behavior for the better.
Other Ways OMT Can Help
In addition to orthodontic issues, OMT can be helpful in resolving a number of other problems. Habitual mouth breathing, for example, can cause trouble for your oral health. Chronic dry mouth (xerostomia) is not only uncomfortable, but also places you at higher risk for developing tooth decay and gum disease. Chronic or obligate mouth breathing—a condition which requires a professional to properly diagnose—is linked to sleep-related breathing disorders and other health problems.
OMT can also help people who have a “tongue tie” (ankyloglossia)—a condition where a small flap of tissue reduces the tongue’s mobility. A minor surgical procedure is often recommended to resolve the issue: using a laser or conventional instrument to snip the tissue will generally release the tongue. An orofacial myologist can diagnose the problem, and provide therapy before and after the procedure to help the tongue regain a full range of motion. Orofacial myologists may also refer their patients to medical or dental specialists for oral problems that are caused by large tonsils, a high, narrow palate, or other anatomical or dental issues.
Orofacial myofunctional therapy can be an effective treatment for many problems in the mouth. Working in conjunction with dentists, orthodontists and medical doctors, orofacial myologists help countless people breathe more freely, eat and speak normally, and enjoy better-looking smiles. If you or your children are experiencing any oral health problems, be sure to tell your dentist about them; he or she can then recommend an appropriate treatment, and refer you for OMT if necessary.

