How Gum Disease Gets Started
The best offense is a good defense against this oral health threat
Who should be concerned about gum disease? Before you say "not me," be aware that gum disease affects almost half of adults over age 30, and 70 percent of adults over age 65. Unfortunately, this condition doesn't always show obvious signs, so millions of people don't realize they have it until the disease reaches an advanced stage. Yet if gum disease is not caught early, it can lead to tooth loss and increase the risk of heart attack and stroke. This merits a look at how gum disease gets started.
Symptoms of Gum Disease
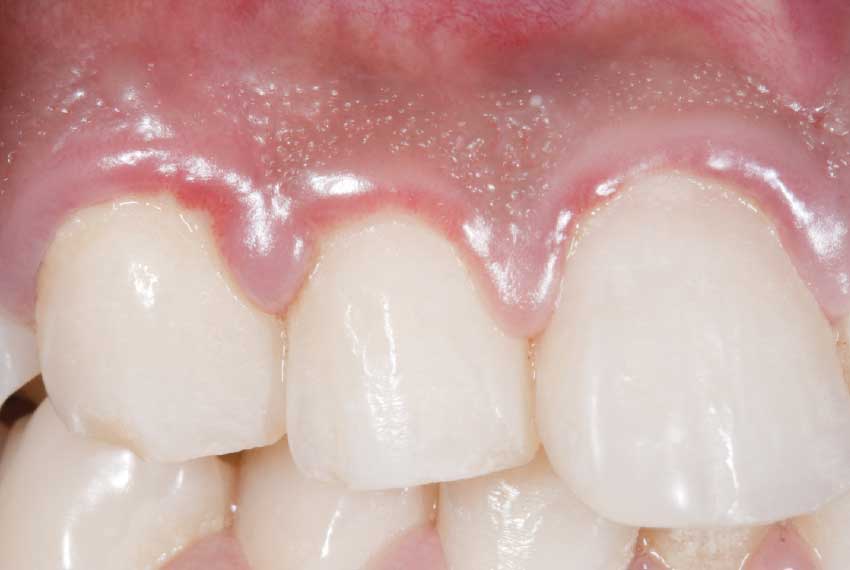 |
| Puffy, reddened gums that will bleed when touched are a sign of gum disease. |
The first stage of the disease is an inflammation of the gums known as gingivitis ("gingiva" – gums; "itis" – inflammation). When gums are inflamed, they can be red, shiny and puffy, and may bleed during brushing or flossing. Fortunately, good oral hygiene and regular cleanings at your dentist's office can turn early gum disease around. However, if gingivitis remains untreated, it can become more serious, progressing to periodontitis ("peri" – around; "odont" – tooth; "itis" – inflammation), an inflammation of the structures that hold teeth in place, and by definition with loss of supporting bone.
Any of the following can be symptoms of gum disease:
- gums that are red, puffy, tender or shiny
- gums that bleed easily when brushing or flossing
- gums that recede or move away from your teeth, making your teeth look longer
- bad breath or a bad taste in your mouth that won't go away
- teeth that are loose or that don't fit together the way they used to
- pus around your gums
If you detect any of these symptoms, make an appointment to see your dentist or periodontist as soon as possible, especially if you have not been for a regular checkup lately.
The Beginnings of Gum Disease
Gum disease gets off to an unremarkable start, beginning with microorganisms that are too small to see with the naked eye. There's no need to get squeamish: We all have millions of bacteria in our mouths, representing hundreds of different species. Most of these bacteria are beneficial, even necessary. They help digest food, keep our gums healthy and fend off many harmful microorganisms. As in other body systems, bacteria help keep the mouth's ecosystem in balance. Only a fraction of the bacteria that live in your mouth are harmful, but this minority can wreak serious havoc on our gums and general health.
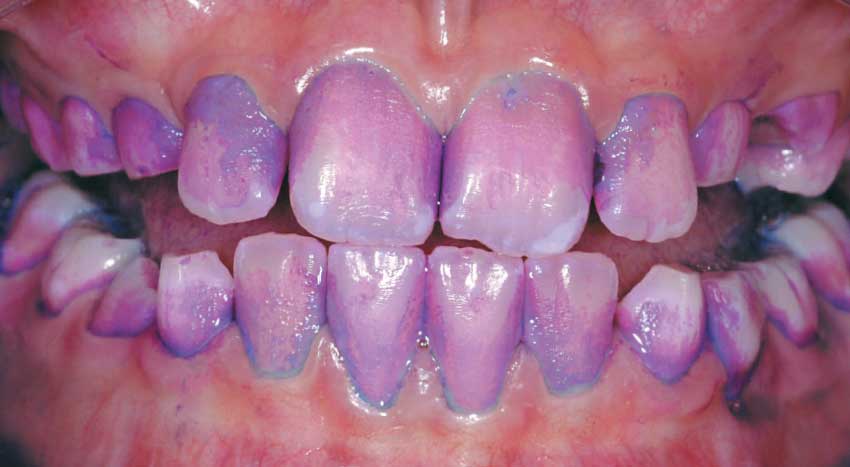 |
| Since bacteria are invisible, a "disclosing solution" is applied to the teeth to identify bacterial plaque. |
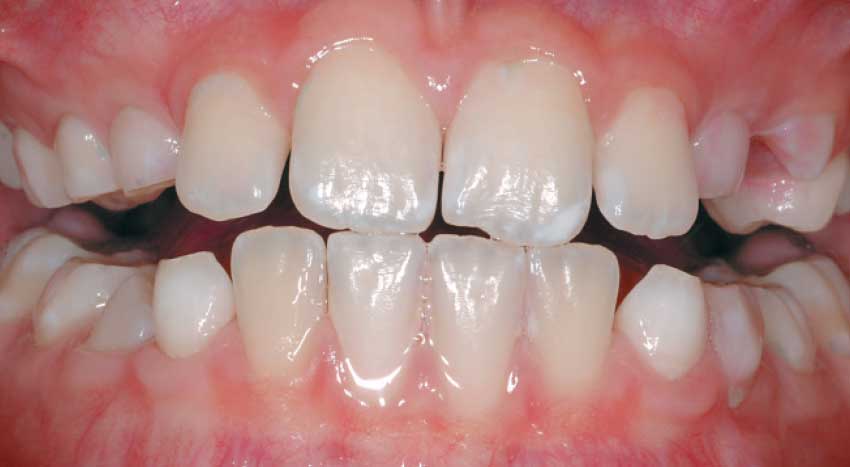 |
| After brushing and flossing, all of the purple disclosing solution is gone, meaning the teeth are clean. |
In the world of bacteria, there is strength in numbers. Some bacteria cells use proteins and other components of saliva to attach to a tooth surface around the gum line, forming a sticky biofilm. A biofilm is more than just a collection of individual bacteria cells; it is an interconnected community of bacteria that forms a web-like 3-D structure. Left unchecked, biofilms become well-organized living systems with channels to transport water and nutrients and remove waste. Further, the cells that make up the biofilm emit chemicals that signal other bacterial cells to join the colony. The sticky biofilm that builds up in your mouth in the absence of effective cleaning is what dentists call plaque.
In its early stages, brushing can keep the plaque from building up on tooth surfaces, and flossing can keep plaque from forming between teeth. But plaque can also form under the gum line, where it is difficult for a toothbrush and dental floss to reach. As plaque spreads below the gum line, the bacteria in the biofilm release toxins, and the body's immune response springs into action to fight off the offending invaders. The combination of toxins from plaque and the chemicals released as part of the body's defense mechanism can start to destroy the bone and soft tissues that support the teeth.
Unchecked Plaque Becomes Tartar (Calculus)
If plaque is not broken up by brushing and flossing, the sticky biofilm — which incorporates the minerals present in saliva — can harden to form tartar, or calculus. At this stage, simple tooth brushing cannot disrupt it.
The plaque and calculus that form below the gum line puts at risk the bone support that secures the teeth in place. As the disease advances, your teeth may become loose, abscesses may form and, ultimately, teeth may fall out. Although regular checkups and cleanings can halt early gum disease and even reverse it, once calculus forms, these hard deposits can be removed only by special cleaning procedures called scaling and root planing, which are performed in a dentist's office.
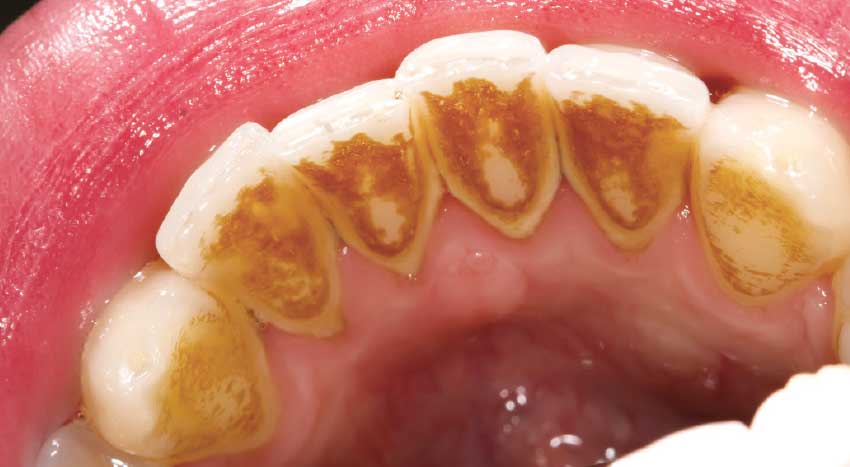 |
| Plaque that is not removed hardens into calculus. |
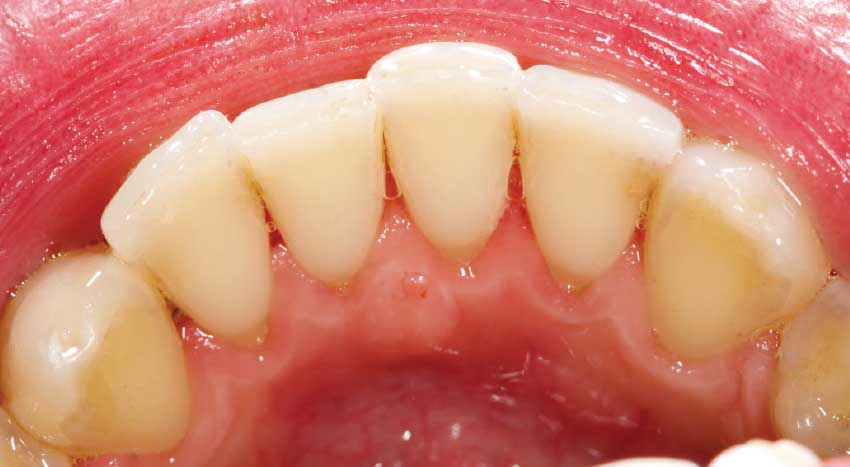 |
| A dental professional, usually a hygienist, is needed to remove all the plaque, calculus and staining. |
If these thorough cleaning techniques do not successfully remove the tartar deposits, surgical treatments may be necessary. Your dentist may wish to refer you to a periodontist, a specialist in dentistry who treats gum disease and is considered an expert in saving your teeth. X-rays will be part of the examination process to determine if the bone surrounding and supporting your teeth has been compromised. If gum disease has caused too much damage, surgery may be needed to regenerate lost bone support and repair oral tissues.
Plaque beneath the surface of the gum tissues is not just a mouth issue. Oral bacteria can enter the bloodstream, triggering inflammation that is associated with many other ills in the body, including cardiovascular disease, type 2 diabetes, lung disease and pregnancy complications. Gum disease is a condition you definitely want to avoid!
What Puts You at Risk of Gum Disease?
Some individuals are at greater risk for gum disease than others because of lifestyle choices, chronic health conditions or heredity. In addition, certain groups of people have a higher incidence of gum disease. These include adults age 65 and older (70.1 percent), people with less than a high school education (66.9 percent), those living below the poverty line (65.4 percent) and men (56.4 percent).
Some people are genetically more predisposed to gum disease — so it makes sense to pay attention to your family history, and monitor your gums more closely if your risk is elevated by heredity. Other factors can make some individuals more likely to get gum disease, including hormonal changes among girls and women, certain illnesses and various medications. People with a compromised immune system due to cancer, chemotherapy, HIV, diabetes and other conditions are more susceptible to gum disease. Diabetes is a double-edged sword — not only can diabetes make gum disease worse; gum disease can lead to raised levels of blood sugar and make diabetes symptoms worse.
Another major risk factor for gum disease is smoking. A significant 64.2 percent of smokers have periodontal disease. Smoking doubles your risk of developing gum disease, and the more and longer a person smokes, the greater the risk. Smoking also weakens the body's immune system, leaving you more vulnerable to the ravages of infection and less responsive to treatment. An added problem is that smoking often masks the symptoms of gum disease like redness, puffiness and bleeding, making it harder to detect. This is because nicotine is a vasoconstrictor ("vaso" – blood vessel; "constrictor" – to tighten), so it reduces blood flow to the gums. Cigarettes are not the only culprit: All forms of tobacco contribute to periodontal disease.
Bad habits like smoking and excess sugar consumption can contribute to gum disease — but so can good habits carried too far, like over-aggressive brushing. Gums can recede as a result of brushing your teeth too hard or too often. Your dental hygienist can show you proper techniques and the right toothbrush to use for optimal tooth and gum health.
What You Can Do
We've seen that among other factors, age, smoking and heredity contribute to gum disease. Since we can't avoid aging or change our genetic makeup, the best way to avoid gum disease is to focus on the factors we can control:
- The first line of defense is your oral hygiene routine at home: Brush your teeth morning and night, using a soft toothbrush and fluoride toothpaste.
- Use an oral fluoride rinse if your dentist recommends one.
- Floss every day.
- See your dentist regularly and have your mouth examined both above the gum line and below it, where a visual exam is not sufficient. The earlier gum problems are detected, the easier they are to treat.
- Have regular professional cleanings to remove tartar and the plaque you can't reach.
- Avoid sugary snacks: The sugar in your food and drinks also feeds the harmful bacteria in your mouth. In fact, sugar has been called "the best fertilizer for pathogenic (disease-causing) bacteria."
- If you have diabetes, manage it well.
- If you smoke, talk with your doctor about quitting.
Gum disease is one of the most common chronic health problems among adults — but it's treatable and, even better, preventable. Being aware of how gum disease gets started is the first step in prevention. In the case of early gum disease, the best offense is a good defense.




